Anatomy Of An Injury, Volume 2
The Overlooked Connection Between Back Pain and Digestion
Muscle soreness following physical exertion is a familiar and expected experience. This discomfort typically resolves after a few days of rest during which time the body repairs minor tissue damage. However, what happens when back pain persists without a clear cause or fails to subside? What other factors can contribute to poor healing?
Identifying the Source
Often, there is a clear moment of injury, a final deadlift, bending awkwardly to pick up a toy, or carrying groceries. These are familiar movements, but fatigue or distraction can cause subtle mechanical errors. Rather than distributing the load through a chain of muscles, a single muscle or isolated portion bears the brunt of the effort, resulting in strain.
But what about the pain that arises without an identifiable incident or fails to heal? When there’s no clear cause to point to, it’s time to consider underlying systems of the body that might be contributing to pain. Nearly ten percent of the global population experiences chronic back pain annually, making it one of the leading causes of disability, missed work, and diminished quality of life. One frequently overlooked contributor is digestive dysfunction. It might seem unrelated, but in my practice, I’ve found a consistent relationship between chronic back pain and impaired bowel health.
The Anatomy of the Gut to Back-Pain Connection
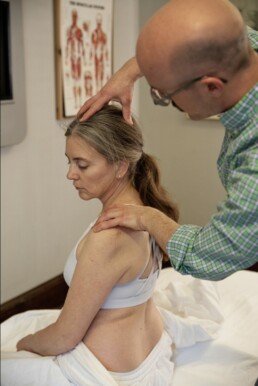
Place one hand on your abdomen over your navel and the other hand on your spine. Notice the depth between your hands. There is significantly more of you in front of the spine than behind it. Beneath your front hand lies skin, subcutaneous fat, abdominal muscles, and layers of fascia enveloping the organs. Deeper still, around twenty feet of small intestine rest against the anterior surface of the spine, separated by the paired psoas muscles. The spine sits far below all of these structures.
The digestive system is inherently dynamic. Food travels approximately thirty feet from the mouth through the esophagus, stomach, intestines, and finally out. This process involves constant, subtle movements that can influence the surrounding tissues. When digestion is sluggish or too fast, aberrant movement along the front of the spine can create stiffness and restrictions that reverberate into the back.
In a healthy body, the fascia is well hydrated and allows for sliding movements without restriction. In the abdomen, fascial sheets between the intestines and neighboring organs, or between and muscles and organs can become restricted. This reduces mobility within the body and leads to a feeling stiff. Over time the health of the spine and vertebral discs suffers from lack of movement. Poor bowel health contributes to overall inflammation which increases our chance of injury and impairs healing.
Assessment and Intervention
When evaluating a client with persistent back pain, I always inquire about digestive health. A healthy bowel pattern is at least one daily bowel movement that is neither too firm nor too loose, passing without strain. Disruptions to this rhythm are common in those with chronic back pain, especially when pain management medications are involved.
As a certified Rolfer®, I assess the tissue quality of the abdomen. Does the belly feel warm and responsive, or cold and sluggish? Are fascial adhesions restricting mobility or placing strain on sensitive nerve tissues? Encouraging movement and awareness in this region can often yield profound changes—not only for digestion but for the spine as well. Emotional factors such as stress, fear, and anxiety also play a role, inhibiting digestion and further exacerbating discomfort.
A Holistic Approach
Recently, I’ve worked with several clients whose primary complaint was long-term back pain. In each case, digestive dysfunction was a significant contributing factor. Rather than focusing solely on the site of the pain, we adopted a front-to-back approach. First, releasing abdominal tension, promoting bowel regularity, and restoring balance to the system as a whole. Once irritation and inflammation subsided we were able to use more direct approaches to address back pain. These clients experienced reduced back pain, improved digestion, and gained understanding about their bodies.
This holistic approach underscores a fundamental truth: the body is an integrated system, not a collection of isolated parts. By addressing the deeper, often hidden contributors to pain, we can achieve more lasting results.
If you’re dealing with persistent back pain, I invite you to consider how your digestive health might be playing a role. Let’s explore how bringing greater awareness and movement to the whole body can support your well-being.
I look forward to working with you at Chattanooga Bodyworks.
Be Well, Eric Maklan
Anatomy Of Healing
Welcome to the inaugural edition of the Chattanooga Bodyworks BLOG: Anatomy of Healing.
In this monthly post, I will share stories of healing from the clinic. Sometimes, we’ll delve into the intricacies of anatomy, while other times, I’ll explore the metaphysical “woo-woo” aspects of life. I’m often surprised by how many new clients begin their story with, “This sounds crazy; you probably won’t understand. No one else gets this…” I want you to know that our human bodies are complex, and your experience is valid. Remember, you are always the expert on yourself. My role is to help you uncover the missing details.
To kick off our blog, I’d like to share a bit of my journey from the past year.
I’m frequently asked what I do when I’m in pain. I like to joke that I go to my maker, referring to the intelligence within this body that built me from a single cell. In practice, I work on myself, doing the movements and exercises I recommend to clients. Additionally, I seek help from other professional when needed (I can’t reach everything!). I believe that health is a team sport.
In a typical year, I expect to be sidelined a few times with significant pain that prevents normal activities, usually lasting no more than a week. For me, this typically manifests as low back or neck pain. However, 2024 was a unique year for my body. It may come as a surprise, but from February to October, I could barely stand. Did I hide it well?
This story began with discomfort at the end of the day while sitting in bed, a burning sensation down my right leg, a typical ‘sciatica’ pain, which is a catch-all term describing pain from the buttock to the posterior leg. This can be caused by nerve compression or muscle tightness. I was uncomfortable but not incapacitated. Then, I staffed a four-day retreat that required me to be on my feet, reliable, and engaged with a group, all while sleeping on an uncomfortable bed, eating unusual food at odd hours, and managing high emotional intensity. I refused to ask to help and stubbornly pushed through. My leg gave out. I was in agony, and that pain lasted for months.
What to do? My body laughed at my usual tricks: movements, stretching, yoga, and breathing. I consulted a physical therapist and diligently followed her routine. I tried a chiropractor and a movement specialist. Despite their expertise, my pain pattern shifted but refused to dissipate. I experienced intense burning in my lower leg, one pain in the morning and another in the evening. I changed my diet and swapped my shoes. I crawled into bed at night, only to crawl out in the morning.
Over the months, I learned to cope with the discomfort. I adapted my movements, allowed myself more time to sit, and slowed everything down. I hibernated in August. Then, at a rock bottom of sorts, I took it back to my maker. I told myself it was not my job to solve the problem. It was not my role to find the magic spot to press upon. Instead of dreading tasks like cutting the grass, I focused on simple activities that would bring me maximum joy. I like jigsaw puzzles, and sitting and moving slowly with stability and support was good for my leg. I reframed my pain from ‘injured’ to ‘healing’. I told myself, “This discomfort is just something I have to go through,” like bad weather on a long hike. I took it one step at a time.
I asked for help more often. I let the grass grow long, held my cat, and discovered ways to stay active without pain. I caution my clients against touching the hot stove; instead, trust that it is still hot. Each test touch is a chance to be burned, extending the suffering. We are intelligent enough to know when the stove has cooled off.
I don’t have a dramatic end to this story. One day, I realized the burning was gone. I reflected on the past week, no pain yesterday or the day before. I had good sleep and a positive mood. Activity that would have caused a flare-up was not an issue. Another week passed, and still no pain. Sometimes, it’s like that. Not all injuries start with a bang or resolve in a clear manner. In hindsight, I am thankful for the experience, my longest stint with serious injury. For now, I look forward to facing more passing trials (ask about my left knee sometime).
If you are struggling with chronic pain (defined as lasting more than six months), please remember: your story is important. Allow yourself to be a part of the healing process rather than defining yourself as injured, hurt, or broken. Words hold power, and the body listens. I listen too. Let’s uncover your story together.